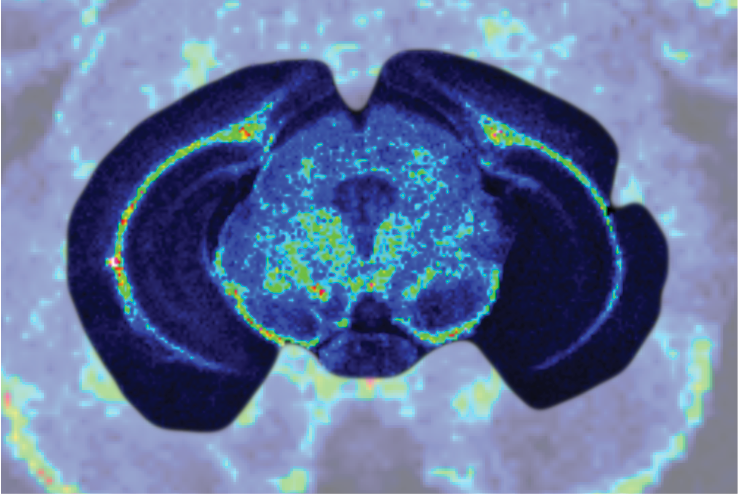
In-vivo imaging to understand biodistribution of a candidate compound
Using imaging in drug discovery
Multimodal and multiscale imaging solutions enable quantification and understanding of organ accumulation and biodistribution, target expression and engagement, optimal biological dose, toxicities/drug interactions and preclinical studies to predict what is seen in the clinic.
Overcoming the challenge of quantitatively determining organ accumulation and distribution at specific time points
In vivo and ex vivo preclinical imaging offers a compelling approach and solution to non-invasively characterise and validate compound distribution and accumulation.
Medicines Discovery Catapult (MDC) has imaging expertise in multi parametric imaging modalities:
- Functional radiological imaging techniques such as positron emission tomography (PET)
- Computed tomography (CT)
- High-frequency ultrasound (HFUS)
- Bioluminescence/near-infrared imaging (NIR)
- ex vivo imaging techniques:
- Mass spectrometry imaging (DESI and MALDI)
- Digital spatial profiler (nanostring DSP)
- Advanced microscopy imaging suite (super resolution/confocal/multiphoton).
How can imaging be used to understand distribution of a therapeutic?
The rate and degree of drug distribution reflects the extent it is present in extravascular tissues and depends on blood flow, capillary permeability, and protein binding. The administered substance goes through a series of cascades to be effective and imaging can track the progress from the systemic level to the cellular level to understand and characterise it.
The 5 steps are:
- Circulation
- Accumulation
- Penetration
- Internalisation
- Release
Examples of imaging techniques that can be used include:
- Fluorescence near infrared imaging device for longitudinal Cy-7 biodistribution. Cy-7 imaging allows deep biological penetration within the body and the ability to image the whole-body distribution with good signal-to-noise. There are many ways to label a molecule with a dye enabling it to be tracked.
- 89Zr PET can also be used to look at whole body distribution and also off target toxicity and nonspecific binding. 89Zr PET is an ideal tracer due to its half-life, allowing repeated images to longitudinally assess distribution of the compound. This technique can also be used to assess tumour penetration longitudinally.
- MDC’s collaboration with the University of Leeds and the therapeutic microbubble consortium in cancer nanoparticles uses an enhanced tumour delivery of microbubbles as a drug carrier in combination with a HFUS platform. Using imaging it can characterise the delivery system and demonstrate that accumulation and distribution of the microbubbles are predominantly through the reticulo endothelial system (RES).
- Three imaging techniques can be used to assess distribution and penetration across the blood-brain barrier (BBB) including PET, near-infrared imaging and bioluminescence probes offer a non-invasive method, and mass spectrometry imaging which has the potential to define drug distribution in very small brain structures with a non-labelled approach.
- Non-invasive mass spectrometry imaging has broad potential in the drug distribution space. Two main mass spectrometry imaging techniques used include desorption electrospray ionisation (DESI) and matrix assisted laser desorption ionisation (MALDI).
Summary
Imaging at MDC offers huge potential as a platform to non-invasively measure the pharmacokinetics (PK) and characterisation of small molecules, biologics and, non-biological complex medicines to facilitate faster translation into clinical development.
This article is based on Juliana’s talk from the MDC Connects webinar series. Watch the session Juliana took part in –Optimising the Compound:

About the author
Juliana Maynard is Lead Scientist in Pre-clinical Imaging at MDC. She works with a wide range of molecular imaging modalities including PET, SPECT, CT and ultrasound. Previously she was Head of Imaging Services at Alderley Imaging and worked at AstraZeneca for 9 years. Juliana has a PHD in neuroendocrinology from the University of Edinburgh.